Introduction
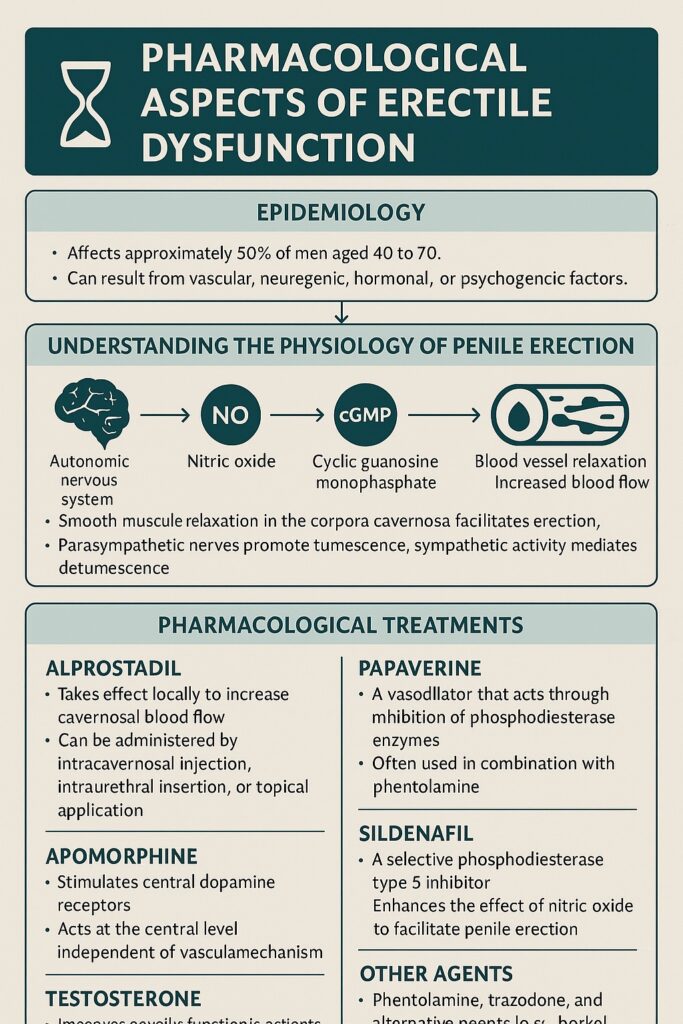
Erectile dysfunction (ED), once euphemistically labeled “impotence,” has moved from the shadows of taboo to the forefront of medical research and therapy. It is no longer dismissed as a psychological curiosity but recognized as a common, multifactorial disorder with profound physiological and psychosocial implications. Prevalence studies demonstrate that nearly half of men aged 40 to 70 will experience some form of ED, with risk increasing in parallel with age and chronic illness. The transition in our understanding — from psychogenic explanations to well-characterized organic causes — has paved the way for targeted pharmacological therapies.
Modern pharmacology has delivered a range of agents that act centrally or peripherally, orally or parenterally, to restore erectile function. Some act as neurotransmitter mimics, others as vascular modulators, and still others address hormonal deficits. This article synthesizes the pharmacological landscape of ED, contextualizing its physiological underpinnings and clinical relevance, while also addressing pitfalls such as drug interactions and contraindications.
Epidemiology and Risk Factors
The burden of ED is considerable. In the United States alone, approximately 10 million men are affected, with ED accounting for nearly half a million outpatient visits annually. While the aging process undeniably contributes, it is overly simplistic to dismiss ED as an inevitable feature of later life. Instead, ED is often the sentinel manifestation of systemic diseases. Cardiovascular disease, diabetes mellitus, hypertension, obesity, and smoking all emerge as significant risk factors.
Equally noteworthy is the role of medications: nearly one in four cases of ED is drug-induced. Antihypertensives, antidepressants, antipsychotics, and endocrine therapies occupy a central place in this list. Thiazide diuretics and β-blockers are particularly notorious, not only for dampening vascular responsiveness but, paradoxically, for depleting zinc — a trace element vital for testosterone metabolism and sexual health.
Psychological stress, depression, and sedentary lifestyle patterns compound these risks, creating a multifactorial network that links metabolic, vascular, neural, and behavioral domains. Early adoption of healthier habits — weight control, smoking cessation, and exercise — has been shown to mitigate ED incidence, underscoring its nature as a partially preventable disorder.
Physiology of Penile Erection
Erection is far more than an isolated hemodynamic event; it is a neurovascular symphony, orchestrated by the interplay of central and peripheral pathways. At its core, penile erection requires smooth muscle relaxation within the corpora cavernosa, leading to increased arterial inflow and restricted venous outflow.
Key players include:
- Autonomic nervous system (ANS): Parasympathetic stimulation facilitates tumescence, while sympathetic activation dominates detumescence.
- Neurotransmitters: Dopamine, norepinephrine, serotonin, and oxytocin modulate central drive, while nitric oxide (NO) serves as the principal peripheral mediator.
- Biochemical cascades: NO activates guanylate cyclase, increasing intracellular cGMP and reducing cytosolic calcium, which in turn relaxes smooth muscle.
The erection cycle itself has been categorized into phases: flaccidity, filling, tumescence, rigidity, and detumescence. Each is marked by precise ANS modulation and vascular shifts. Importantly, phosphodiesterase type 5 (PDE5) hydrolyzes cGMP, terminating erection — a fact that later inspired one of the most celebrated pharmacological breakthroughs of the modern age: sildenafil.
Pharmacological Therapies
The arsenal against ED spans centrally acting dopamine agonists, peripheral vasodilators, hormonal therapies, and PDE5 inhibitors. Below, the principal pharmacologic classes are discussed in detail.
Alprostadil (Prostaglandin E1)
Alprostadil is a synthetic analogue of PGE1, delivered intracavernosally, intraurethrally, or topically. By activating adenylate cyclase and increasing cAMP, it relaxes smooth muscle and enhances cavernosal blood flow. Its rapid pulmonary metabolism minimizes systemic effects, explaining its relative cardiovascular safety. Despite the discomfort of injection therapy, alprostadil remains an effective option for men unresponsive to oral PDE5 inhibitors.
Apomorphine
This centrally acting dopamine receptor agonist works through the hypothalamic and spinal erectile centers, bypassing peripheral vascular mechanisms. Delivered sublingually, apomorphine offers modest efficacy but is hampered by dose-dependent side effects, particularly nausea and dizziness. Its niche lies in patients with contraindications to PDE5 inhibitors.
Testosterone Therapy
Hypogonadism remains a well-documented cause of ED, often accompanied by loss of libido. Testosterone replacement, whether transdermal, injectable, or oral, is reserved for men with laboratory-confirmed androgen deficiency. Importantly, testosterone is not an aphrodisiac; in eugonadal men, it seldom improves erectile performance, though it may enhance mood and desire.
Papaverine and Phentolamine
Papaverine, a non-specific PDE inhibitor, and phentolamine, an α-adrenergic blocker, were among the pioneers of pharmacological therapy. Used predominantly as intracavernosal injections, they induce smooth muscle relaxation and penile engorgement. Combination therapy with both agents yields high efficacy but carries the risk of priapism and fibrosis, relegating them today to second-line use.
Sildenafil and PDE5 Inhibitors
The discovery of sildenafil revolutionized ED treatment. By selectively inhibiting PDE5, sildenafil prevents cGMP degradation, thereby sustaining NO-mediated smooth muscle relaxation. With oral bioavailability and a favorable safety profile, it quickly became the first-line therapy. Headache, flushing, and nasal congestion are common side effects, while co-administration with nitrates remains a contraindication due to profound hypotension risk. Its successors, tadalafil and vardenafil, expanded therapeutic options by varying half-life and onset times.
Trazodone and Other Agents
Trazodone, primarily an antidepressant, can augment libido and prolong nocturnal erections, though its role in ED is limited. Other agents — L-arginine, minoxidil, yohimbine, and herbal supplements such as ginseng and ginkgo biloba — have been investigated with varying success, but they remain outside mainstream recommendations due to inconsistent efficacy and limited evidence.
Drug Interactions and Contraindications
Pharmacological enthusiasm must be tempered by vigilance regarding drug interactions. Sildenafil, metabolized by CYP3A4, has its clearance significantly altered by grapefruit juice, cimetidine, erythromycin, and ritonavir. Conversely, rifampin accelerates its metabolism, reducing efficacy.
The most clinically important contraindication is the concurrent use of nitrates for angina, which can precipitate catastrophic hypotension. Ethanol synergizes with both sildenafil and apomorphine, compounding risks of dizziness and postural hypotension. Alpha-blockers, often prescribed for benign prostatic hyperplasia, can amplify the hypotensive potential of PDE5 inhibitors.
The Future of ED Pharmacology
The pharmacological landscape of ED is evolving rapidly. Research is extending beyond symptomatic treatment toward regenerative strategies — including stem cell therapy, gene therapy, and novel NO donors. Advances in centrally acting agents, improved delivery systems for alprostadil, and combination regimens promise to expand therapeutic efficacy. Importantly, the field is moving toward personalization: tailoring therapy to etiology, comorbidities, and patient preference rather than a one-size-fits-all approach.
Conclusion
Erectile dysfunction, once stigmatized and trivialized, is now recognized as a complex disorder with systemic implications. Its pharmacological management has progressed from crude vasodilators to targeted, well-tolerated oral therapies that have transformed patient outcomes. Yet, treatment extends beyond restoring erections; it restores confidence, intimacy, and quality of life. In this sense, ED therapy embodies medicine at its finest — bridging biology, psychology, and human connection.
FAQ
1. Is erectile dysfunction always related to aging?
Not exclusively. While prevalence increases with age, ED is strongly linked to chronic diseases such as diabetes, hypertension, and heart disease, as well as medication use and lifestyle factors.
2. Can testosterone therapy cure erectile dysfunction?
Only in men with documented hypogonadism. In otherwise healthy men with normal hormone levels, testosterone rarely improves erectile function.
3. Why is sildenafil contraindicated with nitrates?
Both drugs potentiate nitric oxide–mediated vasodilation. Taken together, they can cause dangerous, life-threatening hypotension.