Introduction
Among all urological emergencies, traumatic posterior urethral disruption remains one of the most challenging and consequential injuries. These injuries, frequently associated with high-energy pelvic fractures, test not only surgical precision but also clinical judgment—particularly with respect to the timing and method of urethral reconstruction. Historically, immediate open repair was abandoned due to high rates of incontinence and impotence, while suprapubic diversion followed by delayed urethroplasty became the classic paradigm.
However, the evolving field of minimally invasive endourology has reintroduced an important question: Can endoscopic urethral realignment (EUR), if performed in a deferred but timely manner, reduce stricture length, simplify delayed repair, or even obviate the need for urethroplasty entirely?
The study presented in the provided PDF investigates exactly this question by examining the feasibility, safety, and clinical outcomes of deferred endoscopic urethral realignment in male patients suffering traumatic posterior urethral disruption. Its findings, although based on a select cohort, offer critical insights into how modern urologists might refine their treatment strategies for one of trauma urology’s most complex problems.
The Pathophysiology of Posterior Urethral Disruption
Posterior urethral injuries occur almost exclusively in the context of pelvic fractures. The force that disrupts the pelvic ring transmits energy to the membranous and prostatic urethra, often avulsing the urethra from the prostate. The resulting defect is rarely clean-cut; rather, it comprises hematoma, tissue edema, devitalized mucosa, and an unpredictable degree of distraction.
This pathophysiology is not merely descriptive—it determines outcomes. The longer the gap and the more extensive the surrounding inflammation, the more challenging later reconstruction becomes. Stricture formation is the rule rather than the exception, and the length of the obliterated segment dictates whether a simple anastomotic urethroplasty or a more complex perineo-abdominal approach is required.
The initial goals of management are simple in concept: stabilize the patient, allow hematoma resolution, and ensure urinary drainage. Yet beneath this simplicity lies clinical nuance—whether to intervene early with urethral realignment or simply place a suprapubic catheter and wait months before attempting urethroplasty.
It is within this context that deferred endoscopic urethral realignment aims to strike a balance: not “early” in the classic sense, but not completely passive either.
Concept and Rationale of Deferred Endoscopic Realignment
Deferred (or delayed-early) endoscopic urethral realignment is performed days to weeks after injury, once the patient stabilizes and pelvic hematoma begins to resolve. This timing reduces the life-threatening risks of acute pelvic trauma while targeting an ideal window where inflammation and edema have subsided enough to permit visualization.
The rationale for this strategy includes:
- re-establishing urethral continuity
- reducing the eventual stricture length
- minimizing the complexity of subsequent urethroplasty
- decreasing the likelihood of severe distraction defects
- providing a minimally invasive alternative to open emergency surgery
- potentially allowing some patients to avoid urethroplasty altogether
Critics argue that EUR offers no statistically meaningful reduction in urethroplasty rates and may simply postpone the inevitable. Advocates counter that shorter strictures, less fibrosis, and improved perineal anatomy substantially reduce morbidity associated with later surgery.
The study presented in this PDF contributes valuable evidence to this ongoing discussion.
Study Design and Patient Characteristics
According to the PDF (pages 1–3), the authors prospectively evaluated 34 patients with traumatic posterior urethral disruption managed initially with suprapubic cystostomy. Following stabilization, patients were scheduled for deferred endoscopic urethral realignment.
Key demographic and clinical features include:
- All patients were male.
- Mechanisms of injury were predominantly road traffic accidents (Table 1, p. 2).
- All had posterior urethral injuries confirmed by retrograde urethrography.
- Realignment was performed 7–10 days after injury—timing that allowed hematoma resolution without permitting excessive fibrosis.
- Patients were monitored for stricture formation, urinary continence, erectile function, and need for further intervention.
Fluoroscopic images included in the PDF demonstrate typical pre-realignment findings: complete contrast extravasation and non-opacification of the posterior urethra. These visual cues confirm complete urethral disruption rather than partial tear.
The standardized time window (one week post-injury) represents a crucial methodological element of this paper.
Technique of Deferred Endoscopic Urethral Realignment
The PDF (p. 2) describes the technique in detail, highlighting its reliance on gentle, controlled endoscopic navigation rather than aggressive manipulation.
Step-by-step overview:
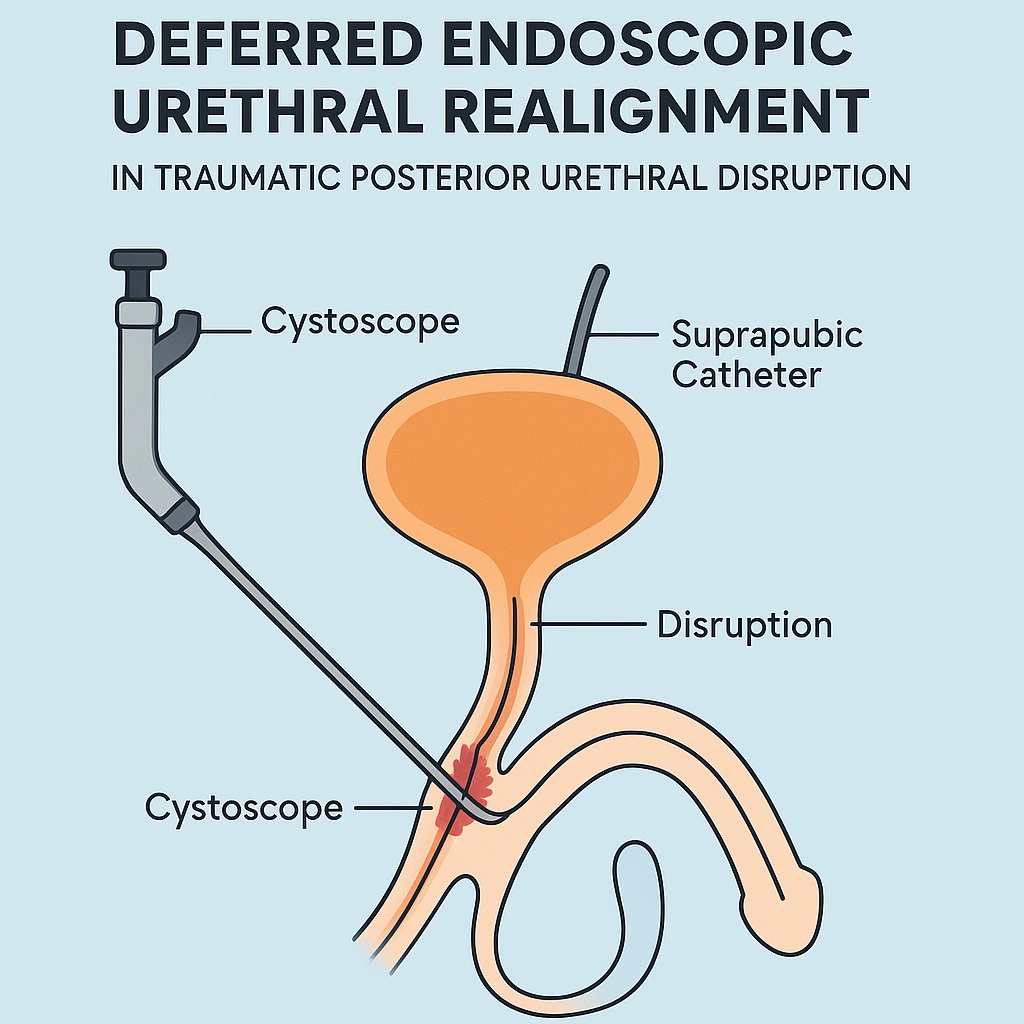
- An antegrade cystoscope is introduced through the suprapubic tract.
- The posterior urethral stump is identified using transillumination and fluoroscopy.
- A retrograde urethroscope is inserted via the external meatus.
- The goal is to establish visual alignment of the two urethral ends.
- A guidewire is passed from one scope to the other, re-establishing continuity.
- A 12–14 Fr catheter is advanced over the wire and left in place for 4–6 weeks.
- Serial imaging is performed before catheter removal.
This technique mirrors modern “rendezvous” endoscopic approaches used in other specialties (e.g., biliary interventions), demonstrating how cross-disciplinary endoscopic principles enhance urological trauma care.
The emphasis on minimal manipulation is deliberate: rough handling risks infection, bleeding, and enlargement of the distraction defect.
Study Outcomes: Stricture Rates and Functional Results
The findings summarized in Table 2 (p. 3) and the results section are critical for evaluating the clinical value of deferred realignment.
Stricture Formation
Despite successful realignment in most patients, stricture formation occurred in 30 out of 34 patients (88%). On first glance, this seems disappointing. But the key lies not in the presence of strictures—nearly all posterior disruptions develop strictures—but in their characteristics.
The majority of strictures were:
- short
- less dense
- amenable to minimally invasive treatment
In fact, 22 patients (approximately 73% of those with strictures) were successfully managed with optical internal urethrotomy (OIU) alone. Only a minority required formal urethroplasty.
This is the most clinically meaningful takeaway: EUR may not eliminate stricture formation, but it simplifies subsequent management, avoiding major open reconstruction in many patients.
Urethroplasty Requirements
Only 8 patients required urethroplasty. Strictures in this group were longer, more fibrotic, or recurrent after OIU.
Urinary Continence
Notably, all patients remained continent, apart from transient stress leakage in two individuals who regained full continence within weeks.
This is significant. Historically, early open repair increased incontinence risk. EUR, in contrast, seems to preserve sphincteric function effectively.
Erectile Function
The PDF reports normal erectile function in 70% of patients. Erectile deficits present in the remaining 30% were attributed not to the procedure, but to the severity of pelvic fracture itself—consistent with established trauma literature.
Thus, deferred realignment appears functionally safe with respect to continence and sexual function.
Interpreting the Stricture Rate: Why 88% Is Not a Failure
The untrained eye may interpret an 88% stricture rate as an indictment of EUR, but experienced trauma urologists know this is expected—and even favorable—given the nature of urethral injury.
Posterior urethral disruptions always heal with fibrosis. The real question is whether surgical intervention later is simple, predictable, and low-risk.
Deferred realignment transforms what could be a 3–5 cm obliterated segment into:
- a 1–2 cm narrowing
- with preserved mucosal bridges
- often treatable endoscopically
In contrast, patients treated with suprapubic diversion alone typically present months later with long, dense obliterative strictures requiring complex perineal urethroplasty.
Thus, EUR’s purpose is not stricture prevention but stricture reduction.
Comparison with Traditional Management Approaches
Traditional management typically follows one of two paths:
1. Immediate open repair (historical approach)
Pros: theoretical restoration of continuity
Cons: devastating rates of incontinence (up to 60%) and impotence
Abandoned decades ago.
2. Pure suprapubic cystostomy with delayed urethroplasty (modern classic)
Pros: avoids acute manipulation
Cons: creates long period of urinary diversion; results in long, complex strictures; requires major surgery later
This method remains widely used, but its disadvantages motivate interest in EUR.
Deferred Endoscopic Realignment
Pros highlighted by this study:
- reduces stricture length
- increases success rate of OIU
- reduces need for major reconstruction
- preserves continence and sexual function
- minimally invasive
Cons:
- still requires specialized expertise
- strictures still form (though shorter)
From a functional standpoint, EUR may represent the optimal balance between intervention and biological healing.
Practical Considerations for Clinicians
The study highlights several practical lessons:
Timing Is Critical
Performing EUR within the 7–10 day window (as shown in this cohort) ensures:
- decreased edema
- improved visualization
- minimized manipulation risks
- reduced fibrosis formation
Patient Selection Matters
EUR is particularly beneficial in:
- hemodynamically stable patients
- those without ongoing pelvic infection
- patients with complete (not partial) disruptions
- patients motivated to avoid major urethral surgery
Imaging Is Essential
Retrograde urethrography and antegrade cystoscopy guide safe navigation. The fluoroscopic images included in the PDF demonstrate typical distraction defects and catheter placement paths.
Endoscopic Expertise Is Vital
The rendezvous technique requires coordinated antegrade–retrograde endoscopy, best performed by experienced endourologists.
Implications for Future Practice
This study adds to growing evidence that:
- pure suprapubic diversion may be overly passive
- immediate repair is outdated
- deferred endoscopic realignment effectively improves downstream reconstructive outcomes
Further multicenter trials with larger populations would strengthen the evidence base. Functional outcomes—particularly erectile function and flow rates—should be tracked longitudinally to evaluate stability over years.
Nonetheless, this paper’s results position EUR not as an experimental strategy, but as a pragmatic, safe, physiologically sound intervention in modern trauma urology.
Conclusion
Deferred endoscopic urethral realignment occupies a unique and increasingly valuable place in managing traumatic posterior urethral disruptions. The technique balances respect for natural tissue healing with timely intervention to prevent extensive fibrosis. While the formation of strictures remains common, these strictures are shorter, less dense, and more amenable to minimally invasive management.
The results of this study—high realignment success, universal continence preservation, majority normal erectile function, and limited need for urethroplasty—demonstrate that EUR is not simply a technical maneuver but a strategic improvement in trauma care.
In an era where minimally invasive approaches increasingly replace open surgical methods, deferred EUR represents a thoughtful re-engineering of urethral trauma management, grounded in anatomy, physiology, and pragmatic surgical judgment.
FAQ
1. Does deferred endoscopic realignment prevent strictures?
No. The goal of EUR is not stricture prevention but stricture minimization. Strictures still form, but they are shorter, less fibrotic, and often treatable with simple endoscopic incision.
2. Does EUR improve continence and erectile outcomes compared to other methods?
Yes. As shown in this study, continence was preserved in all patients, and approximately 70% maintained normal erectile function—rates comparable or superior to traditional delayed urethroplasty pathways.
3. Is EUR suitable for all posterior urethral injuries?
Not universally. The best candidates are stable patients with complete posterior disruptions, without pelvic sepsis, and treated within 7–10 days post-injury by experienced endourologists.